Need Help Now?
Call the Vermont USDA Rabies Hotline at 1-800-4-RABIES (1-800-472-2437) or 1-802-223-8690.
Key Facts about Rabies
- Rabies is a deadly virus that affects the brain and nervous system
- It spreads through bites or saliva from infected animals
- In Vermont, the virus is most often found in raccoons, skunks, foxes, and bats
- Simple steps can prevent rabies, like avoiding wildlife and vaccinating pets
- Rabies is preventable in humans if treated quickly after exposure
- Activity has increased in recent years, with most cases identified in Orleans and Chittenden counties
How to Prevent Rabies in People and Pets
Follow these prevention tips to help keep yourself and your pets safe:
- Do not touch or pick up unfamiliar or wild animals – even baby animals – or try to feed them or make them into pets.
- Make sure trash, compost and recycling bins are tightly closed.
- Do not leave pet food outside.
- Feed pets inside the house and keep pets indoors at night. If they are out during the day, keep them on a leash or within a closed space. Pets that roam free are more likely to be exposed to a rabid animal.
- Make sure that all family pets get rabies shots and keep shots up to date. Animals can be vaccinated by a veterinarian or at a rabies clinic.
Visit the CDC website for more on rabies in domestic animals
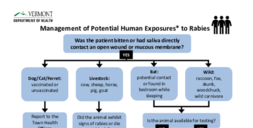
If an Animal Bites You or Your Pet
- Try to capture the animal only if you can do it without getting bitten again. You are more likely to need rabies shots if the animal cannot be found. If the animal is wild, contact the Rabies Hotline (1-800-4-RABIES (1-800-472-2437)) or a Game Warden.
- Wash the bite wound well with soap and running water.
- Contact your doctor and Town Health Officer and follow their instructions.
Call your veterinarian if you believe your pet was exposed to a potentially rabid animal. They will be able to decide if your pet is at risk for rabies and tell you what steps to follow next.
Visit the CDC website for more on rabies exposure
Rabies Vaccine Bait Drop
The Rabies Bait Drop Project is an interstate/international cooperative effort by research veterinarians and wildlife biologists to keep raccoon rabies from spreading across Vermont and the Canadian border. The annual rabies vaccine bait drop generally takes place in August. Early bait drops in May have occurred in recent years to combat rising rabies rates in wildlife.
Vaccine in the form of sweet-scented bait attractive to raccoons and skunks is dropped from aircraft in rural areas and placed by hand in large residential areas. The project's research is directed by the U.S. Department of Agriculture’s Wildlife Services, in collaboration with the Vermont Departments of Health and Fish & Wildlife, and the Agency of Agriculture, Food and Markets.