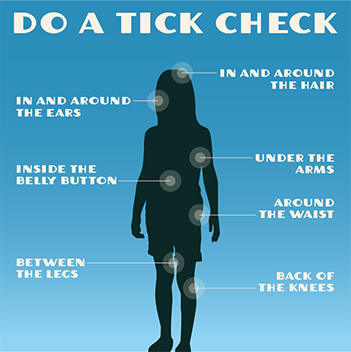
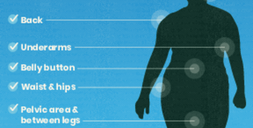
Whenever you spend time outdoors, it’s possible there are ticks nearby. Take simple steps to protect yourself and your loved ones from tick bites and the illnesses they can spread.
Protect
The best way to prevent tick bite illnesses is to prevent tick bites. Before heading outdoors, protect yourself from tick bites:
You can encounter ticks throughout Vermont whenever temperatures are above freezing. Ticks thrive in wooded and brushy areas with high grass, shrubs, and leaf litter. Places like the edges of backyards, farms, trails, and sports fields will likely house many ticks. They’re also found in host animals, like deer, mice, and chipmunks—so you'll likely find ticks wherever you find these animals. Ticks stay low to the ground. They can’t fly or jump– they climb onto animals or humans when they brush by.
Walk in the center of trails (avoiding tall grass and other plants on the edges) to lower your chances of coming into contact with ticks. Mow tall grass or brush in your yard and pick up leaf litter to reduce the number of ticks near your home.
Choose protective clothing such as pants, long-sleeved shirts, long socks, and high boots. Light-colored clothing is easier to spot ticks on.
Consider treating clothing, shoes, and camping gear (NOT skin) ahead of time with 0.5% permethrin. Permethrin kills ticks on contact and gives protection through several washes. Permethrin-treated clothing and gear are also available for purchase.
Choose an Environmental Protection Agency (EPA)-registered insect repellent as these are guaranteed to be safe and effective at preventing bites. EPA has a search tool that can help you find which product will best suit your needs based on how long you will need protection, if you need protection from ticks, mosquitoes, or both, and which active ingredient you prefer.
Insect repellents containing DEET, picaridin, IR3535, Oil of Lemon Eucalyptus (OLE), para-menthane-diol (PMD), and 2-undecanone are most effective against ticks. Always follow product instructions. Avoid repellents containing OLE and PMD if your child is under three years old.
Pets like dogs and outdoor cats can bring ticks into your home. People with pets are more likely to be bitten by a tick and develop a tick-bite illness.
If you have a pet, talk with your veterinarian about tick-prevention products, such as chews, ointments, and collars. Be sure to check your pets thoroughly for ticks after being outside.